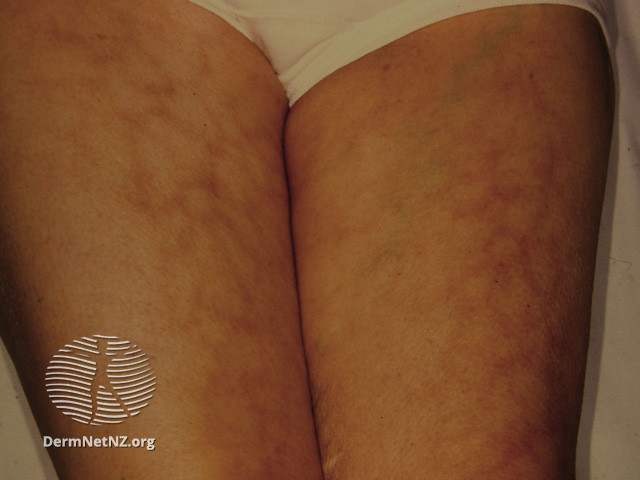
Atopic dermatitis or eczema is a chronic inflammatory skin condition characterised by recurrent acute flares of erythematous (red) itchy skin rash with all without some oozing.
Atopic eczema (AE) usually starts in infancy (< 1 year) or during childhood. Some children outgrow the disease while for maturity it may persist into adulthood. AE can also present for the first time in adulthood
It is estimated that approximately 2.3 million people worldwide suffers from AE. The number of cases is increasing globally including in Asia. Though AE has a lower prevalence in India compared to other Asian countries, the prevalence has consistently increase over the years.
How does one develop AE?
AE is cause by numerous factors interplaying with each other.

How does Atopic eczema presents?

Itching is a hallmark feature of atopic eczema. Itching can worsen the rash or even trigger the onset of eczematous rash.
For this reason atopic eczema is rightfully termed as an “itch that rashes“
Itching in atopic eczema patient can become chronic, lasting for >6 weeks. Scratching to relief the itching can set in motion a viscous itch scratch cycle.
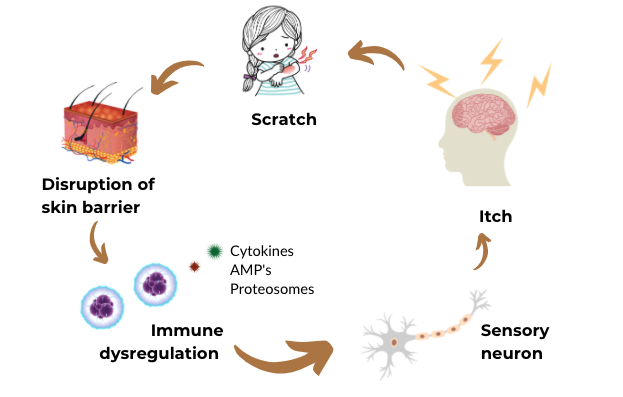
Atopic dermatitis is more than just skin deep?
The damaged skin barrier in patients with atopic dermatitis/eczema allows various allergens (proteins able to mount an immune response in the skin, body) to penetrate the skin, thereby sensitising an individual and causing allergic immune response seen clinically as red itchy rash.
Similar process can occur in the lining of the nose, pharynx predisposing patients to be sensitised to inhaled allergens such as pollen, pollution, dust etc resulting in Allergic rhinitis and or Bronchial Asthma.
A follow up article on the treatment and skin care measures for atopic eczema will be posted in the next blog post.
Atopic eczema in skin of colour
Prevalence of atopic eczema has been reported to be higher in individuals with skin of colour. However the clinical presentation of AE in darker skin tone is different from AE in Caucasians.


Erythema (redness) is usually masked in darker skin tone individuals. Other presentation or associated features are hyperlinear palms, prurigo nodularis, peri orbital melanosis (dark circles), lichenified lesions (thickened hyperpigmented skin) etc.