As I was growing up I’ve seen my mum and most of my aunts trying in vain every remedy available for the pigmentation on their face
What is melasma?
Melasma also called cloasma is a common acquired hyperpigmentation disorder affecting mostly women in their reproductive age groups (~15-45 years) . It is the most common pigmentation disorder & is seen more commonly especially in individuals with darker skin type (FST IV-VI) affecting 9 -50% of the such high risk population . (Find out your skin type here)
What causes melasma?
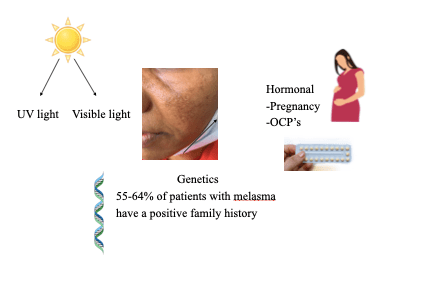
- Genetics: Certain genes are responsible for up regulating enzymes in the melanogenesis pathway (process of melanin production) which results in more melanin production.
- UV Rays: Increase production of reactive oxygen species, which can then increase tyrosinase activity.
- Hormones: Estrogen can up regulate enzymes (tyrosinase) and genes in the melanogenesis pathway, resulting in increase pigment production in genetically predisposed individulas.
How does it present?
Melasma presents with tan brown reticulate (lacy) pigmentation described in three distinct pattern on the face.
- Centro facial pattern: Most common pattern affecting the forehead, nose, upper lip, chin and cheeks
- Malar pattern : As seen in the below images affects the malar area (cheeks) of face
- Mandibular pattern: Affects the jawline and chin, mostly seen in late onset melasma
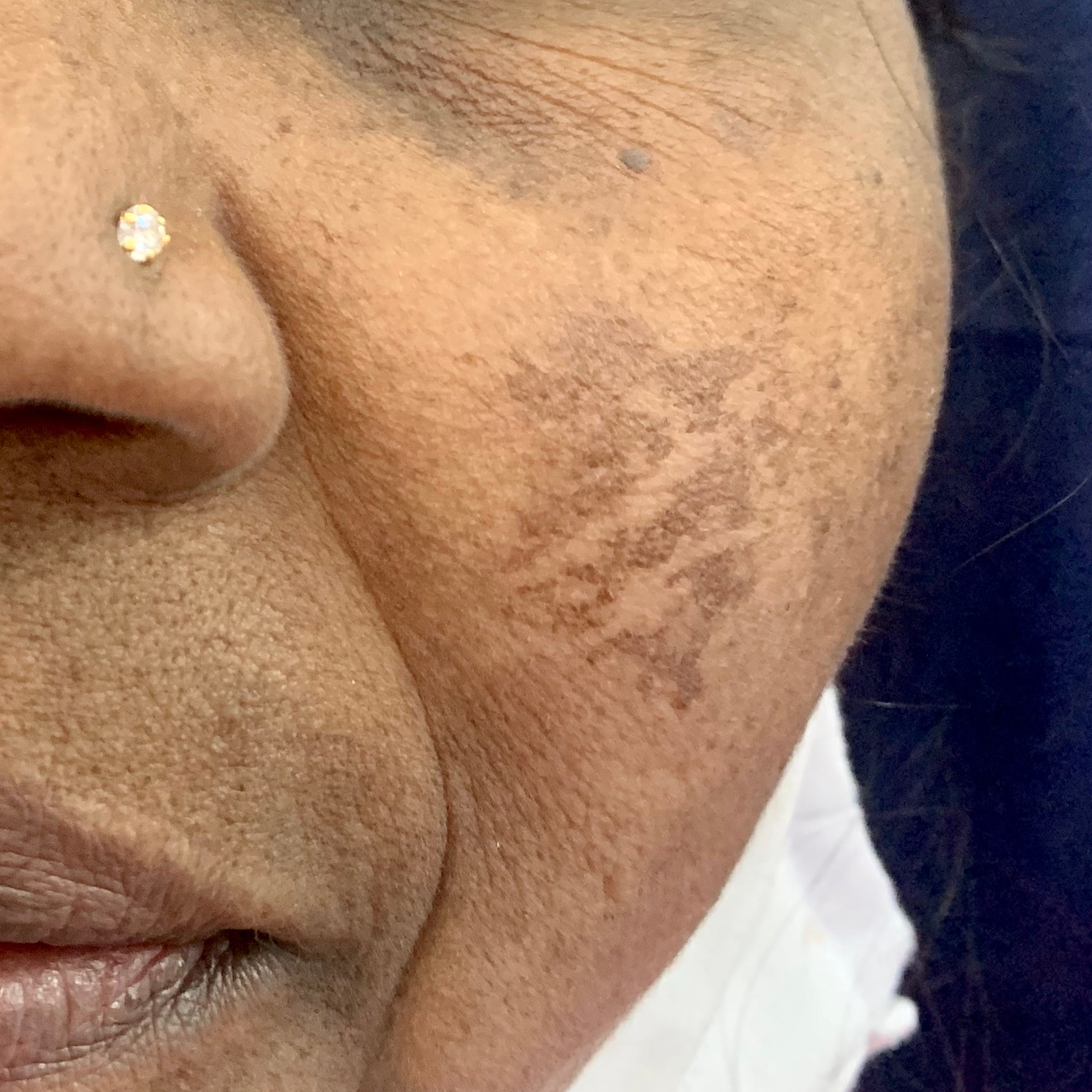

Melasma in women can present for the first time in pregnancy and its referred to as “Mask of Pregnancy“. Treatment of which is more difficult because of the increase estrogen level in the body and as most medications used for pigmentation may not be safe during pregnancy.
The good news is that in some women, this mask of pregnancy is transient and will fade with time and proper management.
Can melasma occur in males?
Yes, melasma can occur in males as well. The male to female is ratio 1:9 i.e for every 9 females with melasma, 1 male individual also suffers from melasma. It has also been reported to have a higher prevalence in Indian males compared to Caucasian males.
Does melasma occur elsewhere besides the face?
Yes, rarely it can involve the neck, chest, the upper arms or forearms and it’s called “Extra facial melasma”
How is it diagnosed?
Most of the time a dermatologist can diagnose melasma by just examining it.
A wood’s lamp examination may be used to assess the dept of the pigmentation i.e if it is epidermal (superficial) or dermal (deep) pigmentation. Epidermal pigmentation respond to treatment better.
Occasionally a skin biopsy (examining of a skin sample under a microscope) may be required for a definitive diagnosis as all facial pigmentation is not melasma.
Treatment options
The hunt for the cure for melasma is still ongoing.
Though numerous treatment options are available now, there is still no “one product” that does it all.
The mainstay of treatment is avoiding the factors responsible for it as much as possible. Since one cannot change one’s genetic makeup, taking measures to avoid the modifiable factors (such strict sun protection) will help prevent its occurrence and reduce the appearance of an already developing melasma.
Its always good to know your personal risk of developing melasma so as you can actively prevent it from occurring in the future.
If melasma is highly prevalent in your ethnic group (for eg: melasma is highly prevalent in my hometown i.e Shillong, Northeast India) start taking preventive measures at the earliest. Its best to consult a dermatologist as early as possible at the start of the pigmentation rather than after a trail and error of using multiple self prescribed creams and remedies.
Shillong, though blessed with its hills, rivers, waterfalls and clouds, being at a higher altitude (1525 m above sea level) means it gets more UV rays than lower altitude areas and the cloud cover aids in scattering these UV rays. Understanding these facts will help individuals be more aware of the need of sun protection even in cloudy, pleasant days without the sun shining bright.
The first step to the treatment or prevention of melasma is strict sun protection. No creams, chemical peels or LASERS will effectively work if one is not complaint with this step

Ideal choice and method of a sunscreen application:
- SPF of at least 30 (measure of UVB protection)
- PA factor +++ (measure of UVA protection)
- Gel formulation or matte finish for those with oily skin
- Apply to both face and neck at least 20 mins prior to sun exposure and reapply every 2 hours especially when outdoors
- Sunscreen application should be on all days even when the sky is cloudy or rainy
- Use a sunscreen even when indoors (as glass cannot filter UVA light)
Other measures of sun protection include using a wide brim hat during your outing tot he beach or during any outdoor activity.
Avoid the peak hours of the day such as between 12 noon -2 pm when the sun is directly above the earth.
Seek shade whenever possible
Treatment to reduce pigmentation
Now that we’ve had sun protection covered, you will need to seek expert opinion (dermatologist) for further management as there are many active ingredients available for treating pigmentation and not everything is suitable for everyone.
If you are on medications such as oral contraceptive pills containing estrogen or drugs for seizures such as phenytoin which could be the potential cause of the melasma, then its best to speak to your treating physician for a possible changeover of the medications.
What are the treatment options available?
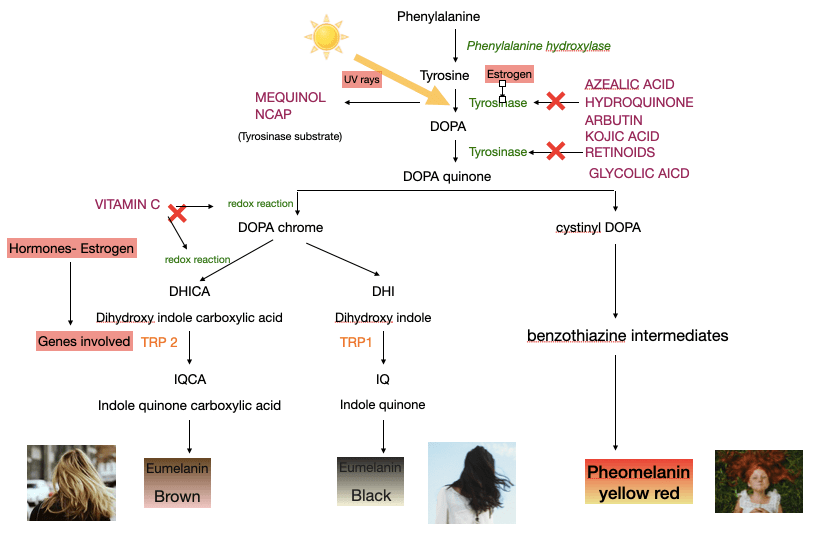
To understand how the treatments work, we first need to have an overview of how melanin (pigment responsible for our skin, hair, eyes colour) is formed.
Topical medications for melasma
Various options are availabe in the form or creams, ointments or serums and the choice will differ from patient to patient.
Topicals required long term and consistent use for the best results.
Not every option will work for everyone
Some of the active ingredients that are use to reduce pigmentation are enumerated in the tables below:
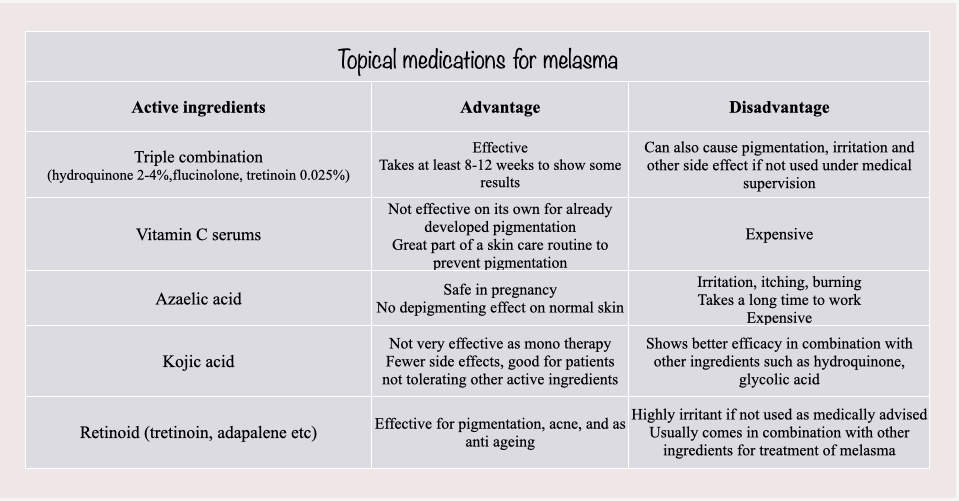
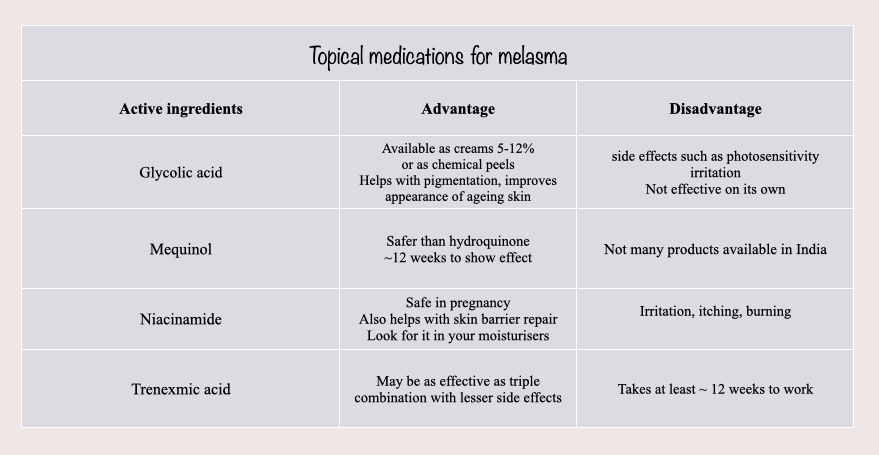
There are numerous options for the treatment of melasma, and the choice will depend with every patient.
For best results, sun protection, strict compliance and abundance of patience is required as improvement can only be appreciated after months of consistent skin care routine.
Oral medications for melasma
Trenexamic acid – An anti fibrinolytic drug that prevents the breakdown of protein (fibrin) present in blood clots. Therefore it is traditionally used to treat bleeding disorders.
It has been shown to be effective for the treatment of melasma in low doses. It has been show to produce results in 3 months but relapse rates are high and melasma recurs within 3 months of discontinuation of the drug.
Side effects are nausea, vomiting & serious side effects such as heart attacks, blood clots in veins of legs, renal injury (kidney problems) could potentially occur in individuals at risk.

Chemical peels
Dermatological procedure where acids of higher strength is used such as glycolic acid, salicylic acid, trichloroacetic acid etc are applied to the face or pigmented area by a dermatologist for a short contact time.
The procedure is done every 3-4 weeks for 5-6 sessions depending on the patient’s response.
Second line treatment for those not responding to topicals alone.
Expensive and requires an experienced hand.

LASER for melasma
Various types of LASER are available for the treatment of melasma.
LASER treatment can be tricky especially in individual’s with darker skin type as the risk of pigmentation is higher. LASER are usually reserved for resistant cases not responding to the above mentioned treatment options.
LASER are not one time treatment. Creams and sunscreens will still be required to maintain the result and prevent recurrence.
LASER treatment are expensive but may be worth it when done by experienced hand.
There is still no cure for melasma.
Seek guidance from a dermatologist as the appearance of the pigmentation can be improved with either depigmenting creams & sunscreens or a combination of treatment especially when the treatment is started early.
